Much has been reported in the media on the ongoing unfortunate deaths of children in the “litchi belt” of Bihar due to Encephalitis – from sensible articles by researchers to the hysterical yet disgusting antics of some media persons barging inside hospitals and harassing on-duty personnel. This article attempts to bring clarity to this issue by laying down the facts that are known with regard to the cause of these illnesses and making some suggestions that can help solve this problem.
What is Encephalopathy/Encephalitis?
Encephalopathy is a broad term for conditions that can cause brain disease, damage, or malfunction. The symptoms of this disorder range from minor memory loss to severe illness such as seizures, loss of consciousness and death. “Encephalitis” is a more specific term for swelling (inflammation) of the brain and is usually caused by viral infections.
The highest concentration of encephalopathy cases in the current outbreak is being treated in Muzaffarpur district of Bihar. This does not strictly mean that all victims are from that district, as these children have also brought to Muzaffarpur from East Champaran, West Champaran, Sitamarhi, Sheohar, Vaishali, and Samastipur districts. Manoj Kumar, Executive Director of Bihar’s State Health Society has been quoted as saying that eleven children with AES have so far been admitted at government health facilities in Samastipur and Vaishali each and six cases are admitted in East Champaran.
Causes of Encephalopathy/Encephalitis?
The cause of AES is unknown in half of all cases across the state. However, in the outbreaks of encephalopathy at Muzaffarpur, the vast majority of cases have not shown any evidence of an active infection. As per health authorities, in the current outbreak in Bihar, Japanese Encephalitis virus has been identified in only two out of over 340 reported cases, thereby raising suspicion of the cause in the vast majority of cases being a toxin rather than an infection.
In studies conducted during outbreaks of AES at Muzaffarpur in June 2011, no viruses or other micro-organisms were identified in the clinical samples of cases presenting with AES, and the absence of isolated organisms has been a consistent feature of AES in the “litchi belt” over the years.
Do litchis cause Encephalopathy/Encephalitis?
The “litchi causes brain swelling” theory may sound almost unbelievable to a layperson, but in medical science, it is well-known and well-documented. A landmark study of 2014 published in the prestigious medical journal Lancet documented the presence of the toxin methylenecyclopropylglycine (hypoglycin A), in the blood samples of children suffering from encephalopathy in Muzaffarpur, which happens to be the highest producer of litchis in the country and supplies over half of the entire litchi business of the state of Bihar.
Hypoglycin A occurs naturally in litchis, and the outbreak of cases too was localised to the “litchi belt” and occurred at the time of harvesting. The researchers further found a strong correlation with children sleeping on an empty stomach after consumption of litchis with the occurrence of the disease. The presence of severe hypoglycaemia (low blood sugar levels) is also well documented in these children, most of whom also had stunted growth parameters suggesting malnutrition.
Administration of 10% glucose IV rapidly reverses the symptoms if given in a time before brain damage sets in. Malnutrition depletes glycogen stores in the body, leaving the child vulnerable to toxin-induced hypoglycaemia which will not usually occur in normal persons with adequate reserves and hence malnourished children are at risk for this condition.
Similar epidemics have been found in other countries with litchi plantations. A research paper published in 2014 pointed out that the presence of hypoglycaemia with the occurrence of AES in Bac Giang Province in North Vietnam coincided with the litchi harvesting season.
AES cases were also reported from Malda district of West Bengal in June and many of the affected children were found to have visited litchi orchards. Hypoglycin was first isolated as the agent that causes “Jamaican vomiting sickness” characterised by a sudden onset of vomiting several hours after a meal containing unripe ackees, followed by the development of severe hypoglycaemia causing convulsions, loss of consciousness and death. Ackee is the national fruit of Jamaica and belongs to the Sapindaceae soapberry species, which is the same family as litchi. As has been noted in Bihar, this disease too occurred mainly in malnourished children.
Even though the researchers who conducted the Lancet study stopped short of categorically labelling the cause as litchi-induced due to the causation-correlation fallacy, they did point out that the most likely cause was hypoglycin A as it satisfied 7 out of 9 points needed for proof of cause. They suggested several remedial measures including restriction of litchis to children and giving the children a proper meal at bedtime, which was implemented by the Bihar government through various local programs.
Subsequently, the incidence of deaths due to encephalopathy showed a strong fall from 2015 onwards and reached single digits by 2018. In 2018, the Bihar government also released a Standard Operating Procedure Manual for Encephalopathy/Encephalitis, which indicates that the government was taking this problem seriously as late as last year.
It is still unclear as to what led to the sudden resurgence in cases this year, with over 340 cases and over a hundred deaths already reported, and whether the surveillance and prevention mechanisms put in place became complacent due to the drop in the number of cases from 2015 onwards.
It has been speculated that several victims were suffering from heat stroke due to the unprecedented heat wave this summer. It is unclear at this point whether the heat wave played the role of an aggravating factor that led to a much higher incidence of cases by causing dehydration in the children who, already being malnourished, were pushed over the edge by the toxins in the fruit. Detailed epidemiological studies will be needed and one hopes adequate blood samples are being collected for later study by the authorities.
Malnutrition in Bihar
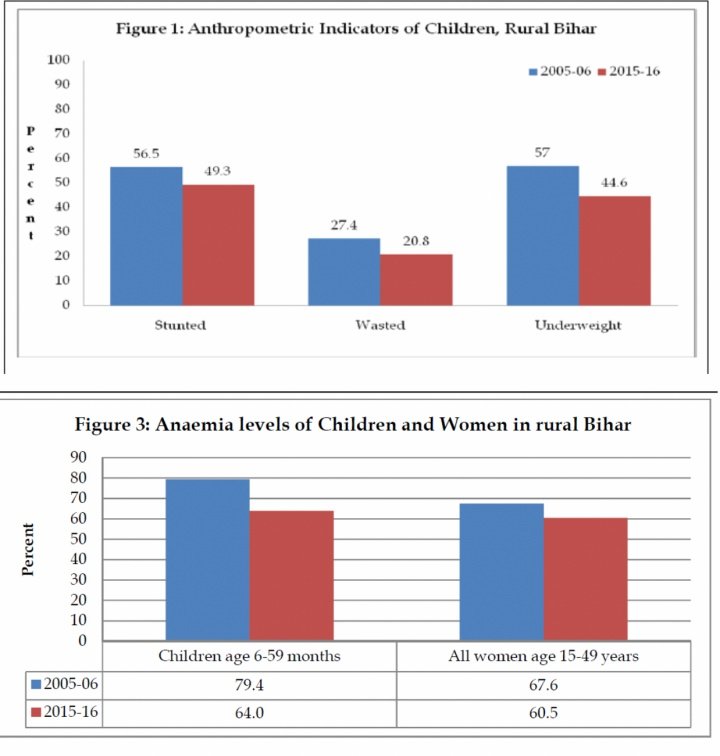
Bihar is one of the worst performing states with regard to childhood and adult malnutrition. According to official data, 49.3% of children are stunted, 44.6% are underweight, and the incidence of anaemia is as high as 64%, which though a significant improvement from the situation a decade earlier, is still extremely high.
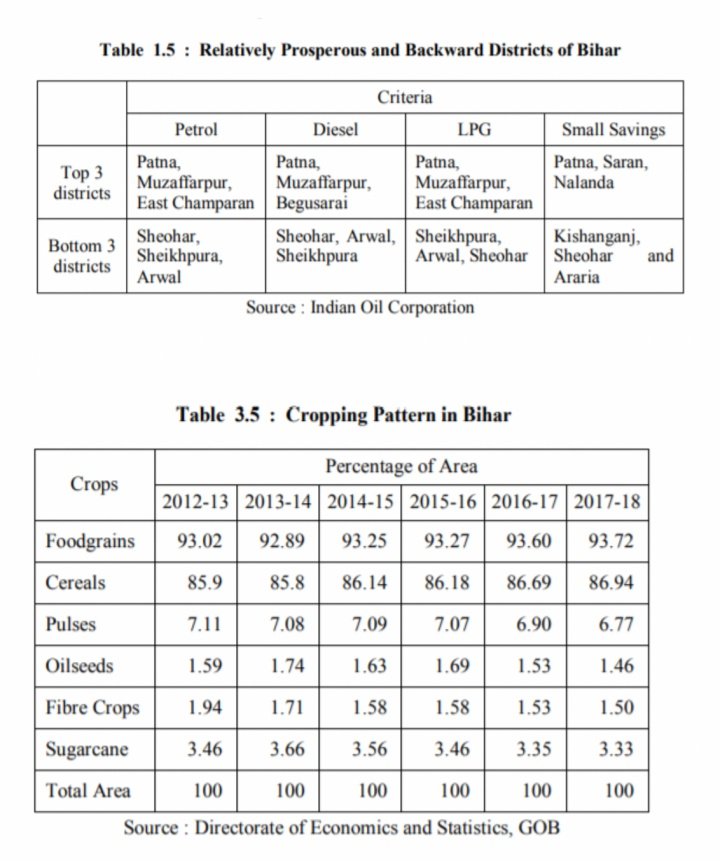
However, Muzaffarpur is one of the relatively prosperous districts of Bihar and is in the top 3 GDP districts of the state as per the Economic Survey 2019 Report. Studies of the average level of food intake in rural Bihar have shown that with respect to cereals, the average monthly per capita intake was 12.13 kg, which is on par with the required dietary allowance (RDA) of 12 kg per month, per person. However, the average per capita consumption of pulses and milk in rural Bihar was found to be lower than the national average as well as the daily recommended allowances. Also, as per the economic survey data, the output of pulses has fallen over the past few years while that of sugarcane has sharply increased.
This clearly indicates that poverty and hunger are not the cause of malnutrition as is commonly believed. The imbalance in the diet with over-intake of cereals and deficiency of pulses and milk is most likely responsible for the high incidence of malnutrition in Bihar.
The author of this article works in tribal rural areas of Maharashtra and has observed a similar dietary pattern in children of these villages, and a similarly high incidence of malnutrition.
Conclusion
Though the causes of AES are many, the cause cannot be identified in about 50% of all cases. In the present outbreak, the most likely cause seems to be due to malnourished children consuming litchis that naturally contain a toxin causing severe and acute fall in blood sugar levels, resulting in convulsions, vomiting, unconsciousness and death. It is also probable but not yet studied or proven that the unprecedented heat wave across the country may have played the role of an aggravating factor by causing dehydration.
The sudden increase in the incidence of AES in children of the litchi-belt of Bihar after a consistent decline over the past few years needs to be investigated. Any lacunae in the monitoring mechanism that was put in place to prevent this disease should be rectified immediately to avoid a similar situation from occurring in future.
Malnutrition is an ongoing problem across the country and Bihar has one of the worst records on this front. The cause of malnutrition seems to be imbalanced diet rather than poverty and hunger. A massive program for the education of parents is needed to bring about a change in dietary habits from carbohydrate-overloaded to a balanced meal. This will admittedly be a challenge that will require long-term vision and commitment as behavioural and dietary changes are very difficult to inculcate in the community.
Simultaneously, a litchi-belt-specific program must be conducted in schools and community warning children and adults of the dangers associated with consumption of litchis in undernourished children, and parents must be encouraged to ensure a proper dinner to all children consuming this fruit.