The term ‘polycystic ovarian syndrome’ (PCOS) has been officially changed to polyendocrine metabolic ovarian syndrome (PMOS) following over a decade of international consultation comprising of clinicians, researchers and patient advocacy groups worldwide. “The Lancet” published the new name on 12th May (Tuesday) after it was revealed at the European Congress of Endocrinology in Prague.
According to Professor Colin Duncan of the MRC (Medical Research Council) Centre for Reproductive Health at the University of Edinburgh, the previous term possibly originated when researchers initially examined the ovaries of patients and detected several tiny sacs filled with fluid, reported The Guardian. These sacs are follicles, which are structures that hold an egg. He added that they are not cysts.
Every month, many follicles grow inside an ovary in healthy women. Eventually, one of these mature and release an egg while the others wither away. However, some follicles stop developing in people with this condition and does not mature to form an egg. The symptoms tend to begin in late adolescence, but it’s a multifaceted issue that can impact women in different ways.
The prevalent feature, polycystic ovaries, inspired the misleading moniker, but several specialists maintained that the name of the condition was inadequate and even deceptive. It failed to accurately reflect the range of metabolic, hormonal, reproductive and psychological issues related to the problem by concentrating solely on the ovaries.
Polycystic Ovary Syndrome #PCOS has a new name Polyendocrine Metabolic Ovarian Syndrome #PMOS. The new term finally reflects the full body metabolic and endocrine impact of this condition and may help drive earlier diagnosis and better care.https://t.co/suxqNEuV3m pic.twitter.com/XYbn4qkjS5
— Scott Isaacs (@scottisaacsmd) May 14, 2026
PCOS/PMOS, its origins and implications
PCOS (now PMOS) has long been used to characterise a common hormonal disorder affecting women of reproductive age. At first, it was assumed to be just a reproductive ailment and was known as Stein-Leventhal syndrome at the time. Scientists in the 1980s learned that it was also linked to insulin resistance or the body’s inability to react to normal insulin levels in the blood.
It was then labelled as PCOS in which androgens, responsible for masculine traits, are generated by the ovaries which causes inconsistent or no periods, ovarian cysts, ovulatory dysfunction, acne, irregular ovulation, insulin resistance, inflammation, abnormal blood sugar level, diabetes, hypertension, cardiovascular disease, high bad cholesterol and triglyceride levels, nonalcoholic fatty liver disease, sleep apnea, unwanted facial or body hair, extreme hair thinning or loss, weight gain, fatigue, difficulties with fertility, pregnancy complications and likelihood of endometrial cancer among an assortment of other manifestations.
It also profoundly damages a person’s psychology, leading to depression, anxiety, diminished quality of life and eating disorders. Importantly, all women possess these “male sex hormones” but those with PMOS have an excessive amount. An imbalance between follicle-stimulating hormone and luteinising hormone triggers this overproduction. Furthermore, this odd abundance is exacerbated by additional factors.
The body also creates more insulin in an attempt to compensate for the fact that multiple women with this concern are more resistant to the hormone. Elevated insulin levels also boost testosterone synthesis. “Increased androgens will also make you more insulin resistant and insulin-resistance makes you produce more androgens. So, there is this vicious cycle,” expressed Duncan.
Obesity is another primary factor which results in a decline in the levels of a protein that absorbs extra androgens in addition to being connected to insulin resistance. PMOS also run in families, indicating a significant influence in relation to heredity. This basically involves a variety of genes.
The Rotterdam Consensus is presently used for its diagnosis. According to the premise, women must exhibit two of the three symptoms, including irregular periods, polycystic ovaries and biochemical or clinical signs of elevated androgen concentration, such as extensive body or facial hair and acne. “It means you can have polycystic ovary syndrome without polycystic ovaries, or you can have polycystic ovary syndrome without an irregular period,” Duncan clarified.
It is noteworthy that an estimated 1 in 8 women or more than 170 million women globally, have PMOS. The World Health Organisation projected that between 10% and 13% of women who are of reproductive age suffer from this, which, interestingly, is more prominent in some regions than others. For instance, it is less common in Northern Europe than in South Asia. However, WHO also mentions that over 70% of women who have this disorder are ignorant about it.
The name change and its importance for women’s health
56 academic, clinical and patient associations have been fighting to rename PCOS for the past 14 years. 14,360 further inquiry replies were obtained after an earlier survey. The aim was to pick out a fresh, correct designation over preserving the PCOS acronym or a generic alias. Ovarian, metabolic and polyendocrine were the recommended keywords to centre on to represent the multisystem consequences of the condition.
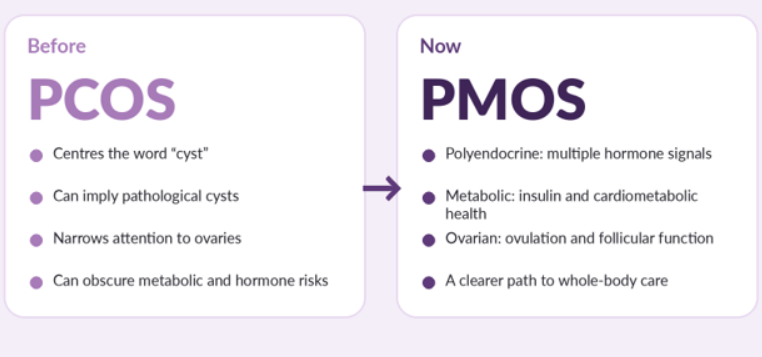
As a result, PMOS was chosen after a comprehensive campaign including 22,000 people in a landmark decision while the symptoms, underlying issues and diagnostic standards remain the same. It stands for — Polyendocrine: Entails several hormone systems. Metabolic: Influences insulin, metabolism and blood sugar control. Ovarian: Recognises the part played by ovaries. Syndrome: A collection of symptoms that frequently coexist.
Not merely an ‘ovary’ issue, not the fault of ‘lazy and fat’ women
Hormones, metabolism, skin, digestion, mental health and the stress response are all sensitive to PMOS, but the entire picture was substantially downplayed when it was reduced to an “ovary” issue. It underestimated the wider scope and instead relied mostly on the ovaries. The recognition that it is a multifaceted condition with endocrine, metabolic, reproductive, psychological and dermatological aspects is evident in the renaming.
PCOS was similarly disingenuous since a lot of women do not genuinely have ovarian cysts regardless of appearance on an ultrasound. However, classifying these cases as such hindered detection and made it harder for patients and medical practitioners to communicate effectively. Hence, patients were dissatisfied with their care.
So yesterday PCOS was renamed to PMOS. After 11 years and about 22,000 people fighting for it.
— khaleesi🧍🏽♀️ (@shelovesore) May 13, 2026
If you’re one of the women who was told to just lose weight or come back when you want children, the reason it was renamed is going to make a lot of things make sense.
Keep… https://t.co/Jm9wa3ZdZ8
Diagnostic criteria and treatment plans won’t be altered right away by the revised classification. Unless there is a need to reevaluate symptoms or dangers to health, current medical methods continue to be valid. Nonetheless, it would be clearer to women that the condition involves key hormonal and metabolic components in addition to the ovaries.
Moreover, it could inspire doctors to take a more complete approach to patient care, stressing screening for blood sugar, cholesterol, blood pressure and other long-term health problems, as well as lifestyle change and interdisciplinary therapy along with reproductive concerns.
Experts mentioned, “By putting endocrine and metabolic in the name, PMOS tells clinicians this is a whole-body condition, not just a gynecologic diagnosis. The new name should help push research toward the metabolic and hormonal roots of the disease, insulin resistance, androgen excess, and chronic inflammation rather than focusing on ovarian cysts. Even though this new name for a long-standing condition affecting women may take some time to associate with PCOS, it is worth the time and patience to better diagnose this whole-body medical phenomenon,” experts mentioned in conversation with Healthline.
Rachel Morman, Chair of Verity PCOS UK (United Kingdom) conveyed, “This shift will reframe the conversation and demand that it is taken as seriously as the long-term, complex health condition it is.” Over the next three years, PMOS will be progressively standardised worldwide and inculcated in 2028 International Guideline update.
Why this is crucial for India
PMOS cases are sharply increasing in India, particularly among young urban women and teenagers. The Indian Council of Medical Research (ICMR)-supported PCOS investigation, is one of the largest in the country, revealed a major regional distinction in frequency and warned of rising metabolic problems within women.
According to a number of findings, estimated incidences might range from 3.7% to more than 22%, depending on region and diagnostic parameters. Scholars have connected the upsurge to sedentary lifestyles and the intake of processed foods, growing obesity, insomnia and stress alongside genetic predisposition.
These women also appeared to be at greater risk for metabolic issues at younger ages. According to a publication in the Indian Journal of Medical Research, almost one-third of Indian women with PMOS have metabolic syndrome. The doctors stated that the latest nomenclature might help divert attention from challenges pertaining to reproduction and stimulate early identification for mental health troubles and cardiovascular disease.
It should support a more interdisciplinary and proactive attitude for care while encouraging early screening for obesity, diabetes, hypertension and other metabolic problems in India.
The renaming might contribute to a reduction in the stigma surrounding the condition
This is a condition of stigmas. According to WHO, the symptoms associated with the condition are socially stigmatised in several settings, damaging relationships with family and friends, job opportunities, a sense of belonging, mental health and other facets of wellbeing. Depression, anxiety, negative body image and issues with socialisation are more usual in the patients.

The stigma is founded on lack of awareness and cultural expectations, especially for female bodies. It is probably experienced differently depending on the specific range of symptoms each person exhibits. These women feel alienated and secluded when they fail to convey their state to the outside world. This is even deemed as a “taboo” because of its correlation with menstruation and the ability to become pregnant.
Basically, a condition that affects the overall endocrine and metabolic health of women throughout their lives, impacts their physical and mental wellbeing, was wrongly confined to just their ovaries, making the whole conversation only about ‘reproductive health’, as if women do not exist beyond their reproductive system, as if women matter only in their reproductive age and not before or after that, as if women deserve to be properly treated only when they are pregnant or trying to be pregnant.
Thus, the new term could aide in lessening the stigma attached to infertility, hair growth, weight gain, acne and hirsutism, boost patient and healthcare provider awareness and facilitate timely recognition.
There’s more to the renaming of PCOS to PMOS than just an adjustment in terminology. It is an embodiment of the expanding scientific knowledge that this is a complicated endocrine and metabolic disorder that affects women’s health for the rest of their lives. It has the potential to raise awareness, mitigate stigma and encourage proactive care in India and abraod where millions of women are undiagnosed or mistreated.
The change of name is a welcome step, because it’s a long-overdue correction that could save millions of women from silent suffering by finally naming the real enemy, and not confining a complex, multi-faceted condition to just ovaries.